“Wow, there were all these people,” recalls Valerie. “Then they put me out, and I don’t remember anything much after that.”
For years, Valerie had been dealing with atrial fibrillation – an irregular heartbeat. She had a pacemaker installed many years ago. But ongoing episodes put her at a higher risk of developing blood clots.
“What happens is blood can become more stagnant inside the heart’s chamber,” explains Dr. Chan. “When that happens, there’s a higher tendency of clots forming inside the heart, and particularly with atrial fibrillation, the clot tends to form inside a location called the left atrial appendage.”
Blood thinners are typically the first line of therapy. But that wasn’t an option for Valerie.
“I have Crohn’s and colitis and diverticulitis too, which can all cause bleeding in the bowel, so I’ve been told not to go on blood thinners,” Valerie says.
Valerie qualified for another option – a minimally-invasive procedure in which Dr. Chan closes off the left atrial appendage permanently.
“I can deploy a device that sits there and blocks off the flow. There will be no blood going in and no clot coming out,” Dr. Chan describes.
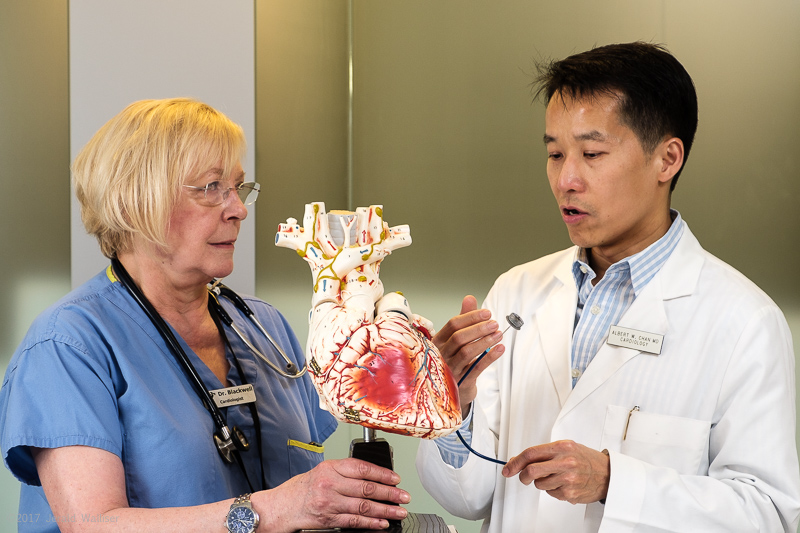
Above: Dr. Margaret Blackwell and Dr. Albert Chan use a model of a heart to discuss closure of the left atrial appendage
Coincidentally for Valerie, the cardiac cath lab had just undergone a donor-funded $3.3 million equipment upgrade. Among the new technology is software that fuses live x-ray and 3D ultrasound to provide real time and comprehensive images of the heart’s structure.
Thanks to donors (and providing an explanation for the number of observers during Valerie’s procedure), Dr. Chan believes Royal Columbian Hospital became the first centre in the country to use this technology to perform a left atrial appendage closure.
“It gives me more information about where the boundary of the appendage is,” says Dr. Chan. “By knowing the location and boundary of the appendage, everything is safer, smoother, there’s less amount of contrast used and it’s quicker to position the device in the right place.”
Valerie says she was out of the hospital the next day and did not experience any pain.
“I didn’t even know there was anything done, really,” she says. “It’s really fantastic what they are able to do with people’s hearts.”